Quiz Results – You Could Benefit From Hormone Replacement Therapy
Your score indicates that you do not have to just "tough it out." Modern, body-identical hormone support is designed to address the root biological cause of your specific symptom profile.
Ready to stabilize your hormones and feel like yourself again? Explore our vetted network of specialists and discover options tailored to your exact needs.
Explore our reviews and comparisons of leading HRT providers
Our top picks for April 2026
What’s Actually Happening to Your Body Right Now?
Symptoms like severe fatigue, vasomotor instability (hot flashes), and cognitive fog are rarely isolated issues, and they are not simply "normal aging." They are clinical markers of systemic hormone decline.
To effectively treat these symptoms, it is critical to understand the biological mechanisms driving them.
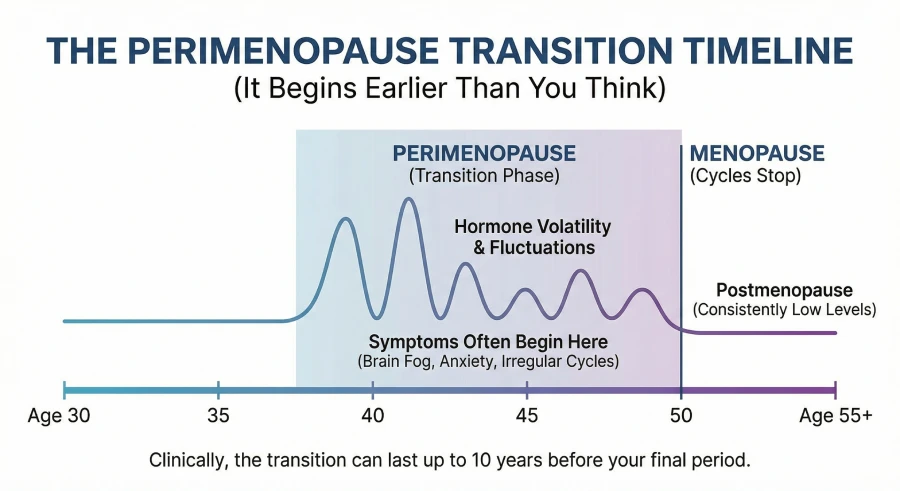
Perimenopause Begins in Your 30s
A primary misconception is that hormone decline begins when menstruation stops. Clinically, the transition phase—perimenopause—can last up to 10 years. Women routinely experience severe hormone fluctuations in their late 30s and 40s. You can be highly symptomatic long before your cycle officially ends.
The Systemic Impact of Hormone Loss
Hormones are not strictly reproductive; they are master metabolic regulators. When the "Big Three" decline, the entire physiological system is disrupted:
- Estrogen: With receptors in the brain, heart, and bones, a drop in estrogen triggers neurological brain fog, vasomotor dysfunction (hot flashes), and a thinning of pelvic tissues.
- Progesterone: As the body's natural neuro-calming agent, dropping progesterone directly correlates with new-onset insomnia, clinical anxiety, and mood instability.
- Testosterone: Women rely on testosterone for musculoskeletal strength and energy. Its decline results in profound physical exhaustion, loss of muscle mass, and a diminished libido.

Metabolic Shifts: Why Caloric Deficits Fail
Sudden weight accumulation around the midsection is a hallmark of menopause. As estrogen declines, the body becomes more insulin resistant and actively redistributes fat storage from the lower body to the abdomen (visceral fat). This is a metabolic shift, not a loss of willpower. You cannot out-diet a biological hormone deficit.
79% of Women Face Medical Dismissal
Statistically, nearly 80% of women must visit a healthcare provider multiple times before receiving appropriate menopause care. Many are incorrectly prescribed antidepressants or told their profound physical exhaustion is "just stress." If your symptoms are impacting your daily function, they warrant clinical treatment, not dismissal.
Hormone Therapy is Preventative, Not Just a Rescue
A pervasive myth is that Menopause Hormone Therapy (MHT) is a "last resort" for unbearable suffering. Medical consensus disagrees. Starting modern hormone therapy early in the menopausal transition is now recognized as highly effective preventative care, actively protecting long-term bone density, cardiovascular health, and cognitive function.
The Clinical Consensus on Safety
Due to misinterpreted studies from the early 2000s, many women hesitate to seek treatment. Today, the medical establishment is clear: Decades of subsequent data prove that for healthy women in their 40s and 50s, modern, FDA-regulated Menopause Hormone Therapy has a well-established safety profile with far more benefits than risks.

Liked this article?

Thank you!